How to Know if Massage Therapy Is the Right Career for You
Choosing a new career can feel exciting, but also overwhelming.
Maybe you’ve been thinking about massage therapy for a while. Maybe you’re burned out in your current job, looking for something more meaningful, or simply curious about working in health and wellness.
Whatever brought you here, one question usually comes up pretty quickly:
“Would I actually be good at this?”
The truth is, many successful massage therapists didn’t start out with experience in healthcare or bodywork. They started with curiosity, a desire to help people, and the feeling that they wanted something more from their work.
If you’ve been wondering whether a career in massage therapy could be the right fit, here are a few signs that it might be.
You Enjoy Working One-on-One With People
Massage therapy is personal work.
You spend your day helping people feel better in their bodies, whether that means reducing pain, relieving stress, or simply helping someone slow down for an hour.
If you enjoy meaningful interaction and like the idea of helping people directly, that’s a strong sign this field could be a good fit.
Many people are drawn to massage therapy because they want work that feels more human and less transactional.
You Want a Career That Feels Meaningful
One of the biggest reasons people choose a career in massage therapy is simple:
They want to feel like their work matters.
As a massage therapist, you see the impact of your work in real time. A client walks in stressed, sore, or exhausted and leaves feeling noticeably better.
That can be incredibly rewarding.
Whether you’re helping someone recover from an injury, manage chronic tension, or simply relax after a difficult week, massage therapy allows you to make a direct difference in people’s lives.
You’re Interested in the Human Body
You do not need a medical background to succeed in massage therapy school.
But it does help to be curious about:
- How the body moves
- Why pain happens
- How muscles and posture affect daily life
A good massage therapy program teaches you anatomy, physiology, and clinical thinking step by step.
Many students are surprised by how much they enjoy learning about the body once they start applying it in a hands-on setting.
You’re Looking for a Career Change
A large percentage of massage therapy students are changing careers.
Some are leaving office jobs that no longer feel fulfilling. Others are coming from industries where stress and burnout have become the norm.
Massage therapy offers something different:
- More flexibility
- More personal connection
- A healthier work-life balance
- The opportunity to do work that feels purposeful
For many people, attending massage school in Seattle is not just about learning a new skill. It’s about creating a different kind of life.
You Like the Idea of Continuing to Learn
Massage therapy is a career where learning never really stops.
After graduation, many therapists continue exploring specialties like:
- Deep tissue massage
- Sports massage
- Injury treatment
- Prenatal massage
- Craniosacral therapy
- Clinical or medical massage
That variety keeps the work interesting and gives you room to grow throughout your career.
What People Often Get Wrong About Massage Therapy
There are a lot of misconceptions about this field.
“Massage therapy is just relaxation massage.”
Relaxation work is part of the profession, but modern massage therapy often includes injury recovery, pain management, and clinical treatment work.
“There’s no long-term career path.”
Many massage therapists build long, successful careers working in clinics, wellness centers, chiropractic offices, private practice, or alongside other healthcare professionals.
“You have to be naturally gifted.”
Like any skill, massage therapy is something you learn through education, practice, and experience.
You do not need to have everything figured out before starting school.
So, Is Massage Therapy the Right Career for You?
Only you can answer that question.
But if you:
- Want work that feels meaningful
- Enjoy helping people
- Are interested in health and wellness
- Want a more flexible and fulfilling career path
…then massage therapy may be worth exploring.
The best way to know is to experience it firsthand.
Take the Next Step
If you’re curious about becoming a massage therapist, visiting a school in person can make a huge difference.
You can:
Sometimes the clearest answers come from stepping into the environment and seeing yourself there.
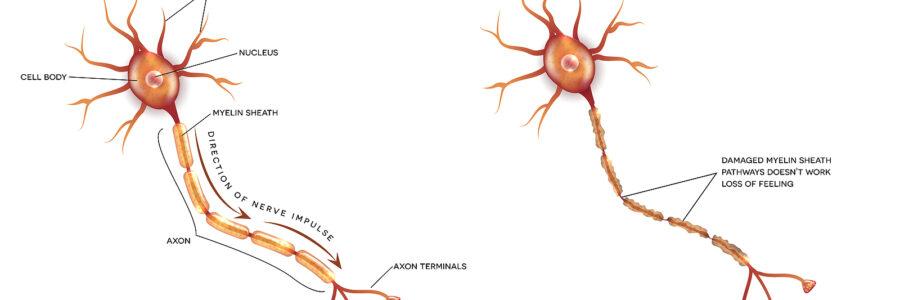
Nerve Damage & Massage Therapy
 Understanding Massage and Its Impact on Nerve Damage:
Understanding Massage and Its Impact on Nerve Damage:
Massage therapy has long been revered for its myriad benefits, from relieving muscle tension to promoting relaxation and enhancing overall well-being. One area of particular interest is its potential impact on nerve damage. While the benefits of massage for muscle-related issues are well-documented, its effects on nerve damage require a more nuanced understanding. In this comprehensive guide, we’ll delve into the relationship between massage and nerve damage, exploring how different massage techniques can aid in nerve repair and provide relief from nerve pain.
Understanding Nerve Damage
Nerve damage, or neuropathy, can occur due to various reasons, including physical trauma, medical conditions like diabetes, infections, and exposure to toxins. Symptoms of nerve damage can range from mild tingling and numbness to severe pain and muscle weakness. Depending on the severity and cause, nerve damage can significantly impact a person’s quality of life.
How Massage Therapy Works
Massage therapy involves the manipulation of soft tissues, including muscles, tendons, and ligaments, to promote relaxation, reduce pain, and enhance overall body function. The primary mechanisms through which massage therapy exerts its effects include:
Improved Circulation: Massage enhances blood flow to the targeted areas, which can promote healing by delivering essential nutrients and oxygen to damaged tissues.
Pain Relief: Through the stimulation of sensory receptors, massage can help reduce pain by blocking pain signals to the brain.
Muscle Relaxation: By alleviating muscle tension and reducing stiffness, massage can improve mobility and decrease discomfort.
Stress Reduction: Massage promotes relaxation and reduces stress levels, which can have a positive impact on overall health and well-being.
Types of Massage Techniques
Several massage techniques can be beneficial for individuals with nerve damage. Understanding the unique characteristics of each technique can help in choosing the most appropriate therapy:
Swedish Massage: This technique involves long, gliding strokes, kneading, and circular movements. It is effective for promoting overall relaxation and improving circulation, which can be beneficial for mild nerve pain.
Deep Tissue Massage: This type focuses on deeper layers of muscle and connective tissue. It can be particularly useful for chronic pain and tension resulting from nerve damage, as it helps release deeply held tension.
Neuromuscular Therapy (NMT): Also known as trigger point therapy, NMT targets specific points of pain in the muscles, which can correspond to nerve pain. By applying pressure to these trigger points, NMT can help release tension and reduce referred pain.
Myofascial Release: This technique targets the fascia, the connective tissue surrounding muscles and nerves. By applying sustained pressure, myofascial release can help alleviate restrictions in the fascia, reducing pain and improving mobility.
Reflexology: Focusing on pressure points in the feet, hands, and ears, reflexology can stimulate nerve pathways and promote relaxation throughout the body. This can be particularly beneficial for systemic nerve conditions like peripheral neuropathy.
Massage Therapy for Specific Nerve Conditions
Different types of nerve damage may respond to massage therapy in various ways. Here are a few common conditions and how massage can help:
Carpal Tunnel Syndrome: Characterized by numbness and tingling in the hands and fingers, carpal tunnel syndrome can benefit from deep tissue massage and myofascial release to alleviate pressure on the median nerve.
Sciatica: This condition involves pain radiating along the sciatic nerve, often affecting the lower back and legs. Neuromuscular therapy and deep tissue massage can help relieve muscle tension and reduce nerve compression.
Diabetic Neuropathy: Nerve damage resulting from diabetes can cause pain and numbness in the extremities. Reflexology and gentle Swedish massage can improve circulation and provide symptomatic relief.
Post-Surgical Nerve Damage: After surgery, nerve damage can occur due to trauma or inflammation. A combination of techniques, including Swedish massage and myofascial release, can aid in the healing process and reduce scar tissue formation.
Considerations and Precautions
While massage therapy can offer significant benefits for individuals with nerve damage, it is essential to approach it with caution. Here are some important considerations:
Consultation with Healthcare Providers: Before starting massage therapy, individuals with nerve damage should consult with their healthcare providers to ensure it is safe and appropriate for their specific condition.
Qualified Massage Therapists: It is crucial to seek massage therapists who are trained and experienced in dealing with nerve-related issues. A qualified therapist can tailor the treatment to the individual’s needs and avoid exacerbating the condition.
Communication: Open communication with the massage therapist is vital. Individuals should inform their therapists about their symptoms, pain levels, and any changes in their condition to ensure the treatment is effective and safe.
Gradual Approach: Starting with gentle techniques and gradually increasing intensity can help the body adapt to the therapy and prevent any adverse reactions.
Conclusion
Massage therapy offers a promising complementary approach for managing nerve damage. By improving circulation, reducing pain, and promoting relaxation, various massage techniques can aid in the recovery process and enhance the quality of life for individuals with nerve-related conditions. However, it is essential to approach massage therapy with careful consideration and professional guidance to ensure safety and efficacy. With the right approach, massage can be a valuable tool in the journey towards nerve health and overall well-being.
For more information about how massage can benefit nerve damage contact our local massage therapy school campus.

Workplace Massage: Boosting Productivity and Employee Satisfaction
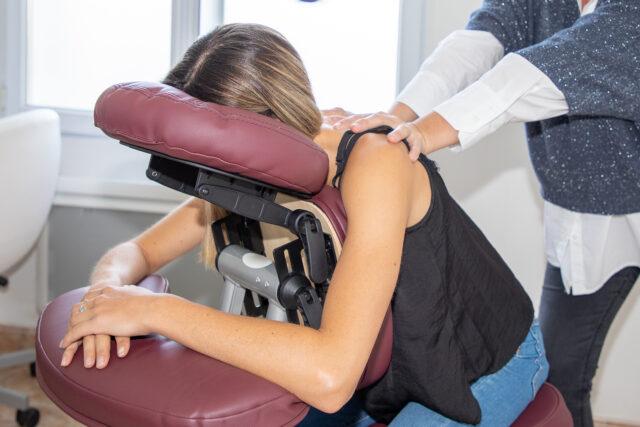 In today’s fast-paced work environments, employee well-being has become a top priority for organizations aiming to create a positive and productive workplace culture. One increasingly popular method to promote workplace wellness is through massage therapy. In this blog post, we will explore how incorporating massage into the workplace can lead to happier, healthier, and more engaged employees.
In today’s fast-paced work environments, employee well-being has become a top priority for organizations aiming to create a positive and productive workplace culture. One increasingly popular method to promote workplace wellness is through massage therapy. In this blog post, we will explore how incorporating massage into the workplace can lead to happier, healthier, and more engaged employees.
- The Impact of Workplace Stress: Workplace stress is a pervasive issue that can negatively affect employees’ mental and physical well-being. High stress levels lead to decreased productivity, increased absenteeism, and a higher risk of burnout. By offering massage as a workplace wellness program, employers can provide employees with a valuable stress management tool.
- Benefits of Workplace Massage: a. Stress Reduction: Massage helps to alleviate stress by reducing cortisol levels and promoting the release of endorphins, the body’s natural feel-good hormones. Regular massage sessions can help employees manage stress more effectively and maintain a sense of calm and balance throughout the workday. b. Pain Relief: Many employees suffer from musculoskeletal issues and chronic pain due to prolonged sitting, repetitive tasks, or poor posture. Massage therapy can target these specific areas, relieving tension, improving circulation, and reducing pain. c. Improved Focus and Mental Clarity: Massage promotes relaxation and mental clarity, which can enhance cognitive function and concentration. Employees who receive regular massages are more likely to stay focused, make better decisions, and perform at their best. d. Enhanced Mood and Morale: Massage triggers the release of serotonin and dopamine, neurotransmitters associated with happiness and positive mood. By incorporating massage into the workplace, employers can create an atmosphere of well-being, boosting employee morale and job satisfaction.
- Different Approaches to Workplace Massage: a. On-Site Chair Massage: Chair massage is a convenient and efficient option for the workplace. It involves a brief, seated massage that focuses on the neck, shoulders, back, arms, and hands. On-site chair massage sessions typically last between 10 to 30 minutes and can be scheduled during breaks or as part of wellness events. b. Wellness Rooms: Creating dedicated wellness rooms within the workplace provides employees with a quiet, comfortable space where they can receive longer massage sessions or engage in relaxation exercises. These rooms can be equipped with massage tables, relaxing music, and essential oils to enhance the overall experience. c. Wellness Programs and Subsidies: Employers can partner with local massage therapists or wellness centers to offer discounted or subsidized massage sessions for employees. By providing financial incentives or flexible schedules to accommodate massage appointments, employers demonstrate their commitment to employee well-being.
- Implementing a Workplace Massage Program: a. Management Buy-In: To successfully introduce a workplace massage program, it’s crucial to obtain support from management and stakeholders. Highlight the potential benefits, present case studies, and emphasize the positive impact on employee satisfaction, retention, and productivity. b. Partnering with Professionals: Collaborate with licensed and experienced massage therapists or wellness providers who specialize in workplace programs. Ensure they understand the unique needs of office environments and are capable of delivering quality services. c. Communication and Promotion: Proper communication is key to the success of any workplace wellness initiative. Use various channels, such as emails, newsletters, posters, and intranet platforms, to inform employees about the availability and benefits of the massage program. Highlight success stories and encourage employee feedback to create a buzz and generate interest. d. Evaluation and Feedback: Continuously evaluate the effectiveness of the program through employee surveys, feedback sessions, and productivity metrics. Adjust the program as needed based on employee preferences and needs.
Massage therapy is a powerful tool for promoting workplace wellness and improving employee satisfaction and productivity. By addressing stress, reducing pain, enhancing focus, and boosting morale, workplace massage programs have the potential to transform the work environment into a healthier, happier, and more efficient space. Employers who invest in the well-being of their employees through massage initiatives demonstrate their commitment to fostering a positive work culture. By incorporating massage into the workplace, organizations can unlock the full potential of their workforce and reap the long-term benefits of a more engaged and productive team.

Lupus & Massage Therapy
 Lupus, also known as Systemic Lupus Erythematosus (SLE), is a chronic autoimmune disease that can affect various parts of the body, including the skin, joints, kidneys, heart, and lungs. The condition occurs when the immune system mistakenly attacks healthy tissues in the body, causing inflammation and damage.
Lupus, also known as Systemic Lupus Erythematosus (SLE), is a chronic autoimmune disease that can affect various parts of the body, including the skin, joints, kidneys, heart, and lungs. The condition occurs when the immune system mistakenly attacks healthy tissues in the body, causing inflammation and damage.
While the exact cause of Lupus is unknown, it is believed to be a combination of genetic, environmental, and hormonal factors. Women are more likely to develop the condition than men, and it often appears between the ages of 15 and 44.
The symptoms of Lupus can vary widely, depending on which part of the body is affected. Common symptoms include fatigue, joint pain and stiffness, skin rashes, fever, hair loss, and chest pain. In some cases, Lupus can lead to more serious complications, such as kidney failure, heart attacks, and stroke.
There is currently no cure for Lupus, but treatment options are available to manage symptoms and prevent complications. These may include medications such as anti-inflammatory drugs, corticosteroids, and immunosuppressants, as well as lifestyle changes such as getting regular exercise, eating a healthy diet, and avoiding triggers that can worsen symptoms.
Massage therapy is one complementary therapy that may help people with Lupus manage their symptoms and improve their overall quality of life. Here are some of the ways that massage therapy can benefit patients with Lupus:
- Reducing Pain and Stiffness: Massage therapy can help reduce muscle and joint pain and stiffness, which are common symptoms of Lupus. Massage can help increase blood flow to the affected areas, promote the release of endorphins (natural painkillers), and reduce inflammation.
- Promoting Relaxation and Stress Relief: Stress can worsen symptoms of Lupus, and many people with Lupus experience anxiety and depression as a result of their condition. Massage therapy can help promote relaxation and reduce stress, which may help improve overall mental health.
- Improving Sleep: Many people with Lupus struggle with sleep disturbances, including insomnia and restless sleep. Massage therapy can help promote relaxation and improve sleep quality, which may help reduce fatigue and improve overall well-being.
- Boosting the Immune System: Massage therapy has been shown to stimulate the immune system and increase the production of white blood cells, which are responsible for fighting off infections. This can be particularly beneficial for people with Lupus, whose immune systems are compromised.
- Providing a Safe and Nurturing Environment: Many people with chronic illnesses such as Lupus may feel isolated or disconnected from others. Massage therapy provides a safe and nurturing environment where patients can feel cared for and supported, which can have a positive impact on their overall mental and emotional well-being.
It is important to note that massage therapy should not be used as a substitute for medical treatment for Lupus. However, it can be a valuable complementary therapy that can help improve symptoms and overall quality of life for people with Lupus.
If you are considering massage therapy as a treatment option for Lupus, be sure to talk to your healthcare provider first. They can help you determine if massage therapy is a safe and appropriate option for you, and can also recommend qualified massage therapists who have experience working with patients with Lupus.
Being a Massage Therapist -10 Benefits
 Being a massage therapist can be an incredibly rewarding and fulfilling career. Not only do you get to help people feel better physically and emotionally, but you also have the opportunity to make a positive impact on their overall well-being. In this blog post, we’ll take a look at the top 10 best things about being a massage therapist.
Being a massage therapist can be an incredibly rewarding and fulfilling career. Not only do you get to help people feel better physically and emotionally, but you also have the opportunity to make a positive impact on their overall well-being. In this blog post, we’ll take a look at the top 10 best things about being a massage therapist.
- Helping people feel better
One of the most obvious benefits of being a massage therapist is the ability to help people feel better physically. Whether your clients are dealing with chronic pain, injury, or just need to relax, your massage techniques can provide relief and promote healing.
- Building relationships with clients
As a massage therapist, you have the opportunity to build long-lasting relationships with your clients. Many people see their massage therapist regularly, which means you have the chance to get to know them on a personal level and help them on their journey towards wellness.
- A flexible schedule
If you’re looking for a career with a flexible schedule, massage therapy is a great option. You can set your own hours and work as little or as much as you want. This can be especially helpful if you have other commitments, such as family or school.
- A variety of work settings
As a massage therapist, you can work in a variety of settings, from spas and resorts to hospitals and clinics. This can provide a lot of variety in your work and allow you to explore different aspects of the profession.
- Continuous learning and growth
There’s always something new to learn in the field of massage therapy. From new techniques and tools to advances in technology, there are plenty of opportunities for continuous learning and growth. This can help you stay engaged and excited about your work.
- A physically active job
If you’re someone who enjoys staying active, massage therapy can be a great career choice. You’ll be on your feet for most of the day and using your hands and arms to perform massage techniques, which can provide a good workout.
- A positive impact on mental health
Massage therapy isn’t just good for physical health; it can also have a positive impact on mental health. Massage has been shown to reduce stress, anxiety, and depression, and can promote relaxation and improve mood.
- A career that’s in demand
As more people become interested in natural and alternative forms of healthcare, the demand for massage therapists continues to grow. This means there are plenty of job opportunities available and a good outlook for the future of the profession.
- The ability to be self-employed
If you’re someone who values independence and autonomy, becoming a self-employed massage therapist may be a good fit. You can set your own rates and build your own business, which can be a fulfilling and rewarding experience.
- Making a difference in people’s lives
Perhaps the biggest benefit of being a massage therapist is the ability to make a positive difference in people’s lives. Whether you’re helping someone recover from an injury, manage chronic pain, or just relax and unwind, your work can have a profound impact on their well-being.
In conclusion, being a massage therapist can be a wonderful career choice for those who are passionate about helping others and promoting wellness. From the ability to make a positive impact on people’s lives to the flexibility and autonomy that comes with being a self-employed massage therapist, there are plenty of reasons to consider pursuing this rewarding profession.
For more information about being a massage therapist contact our massage school admissions team

IT Band Syndrome

Did you know that engaging in activities that involve repetitive flexing and extending of knees can cause iliotibial band syndrome? Well, studies show that walking long distances, cycling and athletics, among others are some of the contributing factors. As a nurse, physical therapist, fitness coach or yoga instructor, you will always encounter clients with IT band injuries. According to experts, incorporating massage therapy with conventional treatment is one of the best approaches to manage IT band syndrome.
What Is IT Band Syndrome?
The IT band is a thick connective tissue that originates from the pelvic bone and extends laterally to the shinbone. The fibrous band works with hip muscles to stabilize lateral movements of the hip and knee. However, overworking the connective tissue with activities that require repetitive knee flexion and extension causes IT band syndrome. The overuse movements create friction between the band and the lateral femoral epicondyle, thus, causing discomfort when exercising, or moving. Signs and symptoms of IT band syndrome include:
- Patient reports feeling an irritating pain along the lateral side of the hip and the femoral epicondyle during motion.
- There is notable inflammation and swelling on the outer part of the knee.
- Slight pain is felt at the beginning of an exercise and increases with intensity as the activity progresses.
- Pain in the gluteal region caused by overstretching gluteus muscles.
- Experiencing a popping pain that results from the rubbing of IT band against your knee during movement.
- Tenderness on the lateral femoral and tibia epicondyles upon palpation
Diagnosing the IT Band Syndrome
Despite causing knee pain, iliotibial band syndrome is not the only cause of knee discomfort. Before making your diagnosis, ensure you take a history of the client’s complaints and their daily activities. Usually, the iliotibial band syndrome affects people who engage in activities that put a constant strain on the knees. A client who reports being a runner, bicyclist, hiker or athlete might be a candidate of iliotibial band syndrome.
After taking the history, the next essential step is to conduct a comprehensive physical assessment to determine the precise effected location. You can use some tests such as Noble’s test to assess for pain in the lateral femoral condyle. Additionally, using an Ober’s test will assist you in examining the IT band for tightness. A comprehensive physical examination will give you an insight on areas that need massage therapy; to determine the appropriate techniques for myofascial release.
Managing IT Band Contracture Syndrome with Massage Therapy
As a professional health worker, ensure that massage therapy is in your to-do interventions for iliotibial band syndrome. Offering a massage along with traditional treatment has proved to be effective in enhancing recovery from the IT band syndrome. Below are the benefits of massaging your patients:
- Relieve Lateral Leg Pain
In most cases, it’s a nagging pain resulting from IT band overuse that forces patients to seek professional intervention. Performing myofascial release massage on the lateral side of the effected leg relaxes the fibrous band and muscles from tension — thus alleviating the pain.
- Promote Healing
Nowadays, unique massage techniques aim to not only relieve pain but also to promote tissue healing. Addressing trigger points and hypertonicities of the leg muscles enhances blood circulation. Improved tissue perfusion allows delivery of oxygen and nutrients to enhance the healing of the injured tissues.
- Restore flexibility and Improve Mobility
A patient who is suffering from IT band syndrome often complains of inability to move comfortably. Massage therapy resolves muscle stiffness and tenderness, therefore refining motion and flexibility. Therefore, after several sessions, your patient will be able to resume daily activities with ease.
- Improve Posture
When the pain is intense, most people adopt bad postures in response to the discomfort. As a massage therapist, you are equipped with unique skills to resolve tension and inflammation of the effected regions. The relaxation and flexibility of the leg enable the patients to assume their normal and healthy posture.
- Alleviate Stress and Anxiety
Besides enhancing physical fitness, massage treatment helps to relieve the body from stress. Reduced anxiety in patients with IT band syndrome promotes healing and improves their emotional well-being.
What is the prognosis of Iliotibial Band Syndrome?
Typically, if you utilize the right treatment modalities, the prognosis of IT band friction syndrome is excellent. For optimum results, it is crucial to use a multifaceted approach when treating patients. Whether you are a nurse, physical therapist, or a fitness coach, integrating massage therapy with conventional treatment will yield a positive outcome.
Ultimately, adding massage therapy to your healthcare profession not only improves healthcare delivery to your clients but also makes you indispensable. Want to learn more about managing IT band syndrome with massage therapy? Contact our Seattle massage therapy schools today to discuss your massage career and educational options in Seattle, Tacoma, or Bellingham.
I addition you can also contact our partner massage therapy school; Seattle Clinical Massage School for information about a massage therapy career in Seattle, Washington.

Degenerative Disc Disease & Massage
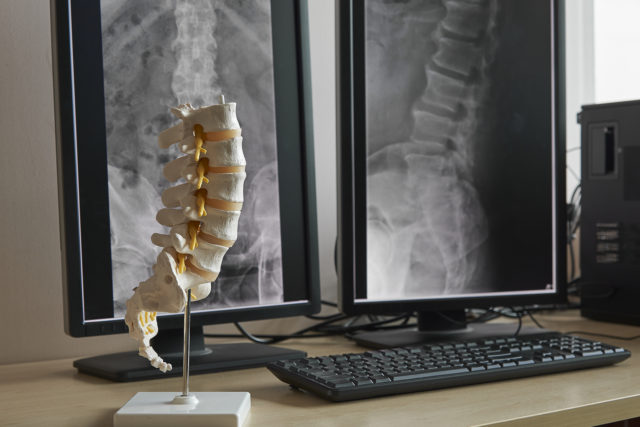
Degenerative disc disease (DDD) is a medical condition where one or more discs in the back lose strength. Despite the name, degenerative disc disease isn’t technically a disease but a progressive condition that worsens over time due to wear and tear, or injury.
The discs in your back are situated in between the vertebrae of the spine and act as cushions and shock absorbers. They help you stand up straight and move through everyday motions, such as bending over or twisting around. As people age, DDD can worsen and cause mild to extreme pain that can interfere with your everyday activities.
Symptoms of Degenerative Disc Disease
Some of the most common symptoms of degenerative disc disease include pain that:
- Primarily affects the lower back
- Could extend to legs and buttocks
- Stretches from neck to arms
- Can be worse from sitting
- Worsens after bending or twisting
- Comes and goes in a few days or extends to several months
People with DDD might exhibit less pain after walking or exercise. Additionally, DDD can cause weakened leg muscles and numbness in your arms or legs.
Causes of Degenerative Disc Disease
DDD is primarily caused by natural wear and tear of spinal discs. Over time, discs tend to dry out and lose their support and function, leading to pain and other symptoms. DDD can start developing in your 30s or 40s and progressively worsen as you age. However, the condition can also be caused by overuse from sports or repetitive activities, or injury. Once a disc is damaged, it can’t repair itself.
Risk Factors
Age is the major risk factor for degenerative disc disease. The discs in between the vertebrae often shrink down and lose their cushiony support as people age. Almost every adult above the age of 60 has some form of disc degeneration. However, not all cases cause pain.
Long-term repetitive activities that place a lot of pressure on certain discs can also increase your risk. Other risk factors include car accidents, overweight or obesity, and a sedentary lifestyle.
Diagnosis of DDD
An MRI can help detect degenerative disc disease. Your doctor may recommend this type of imaging test based on a physical exam or an investigation into your symptoms and health history. Imaging tests can reveal damaged discs and help rule out other triggers of pain. When you receive a diagnosis of DDD, it does not mean that you’re disabled or headed for a downward spiral of spinal degeneration. In fact, DDD is often a part of the natural aging process that we all go through at some point in life. And the good news is that you can mitigate the associated pain through a variety of treatment solutions, including massage therapy.
Massage Therapy Treatment for DDD
From a Massage Therapy point of view, the approach in treating DDD is to strike a balance between reducing muscle tension and enhancing traction (decompressing the targeted vertebral segments). Finding a “green zone” of treatment is critical since the spasms that occur through the neck or low back happen because the body is trying to protect that area. By applying slow, repetitive, methodical massage between soft tissue and joint mobilization (spinal decompression), massage therapy can help relieve pain and allow you to move easier and execute strengthening exercises efficiently.
Massage therapy generally helps in these three ways:
- Increasing Blood Flow and Circulation: Proper blood circulation ensures that critical nutrients flow back fully to the strained muscles and tissues. This makes the muscles/tissues stronger, helping relieve the strain coming from the degenerating discs.
- Decreasing Tension: The muscles can become tense as they struggle to compensate for the weakening discs. When these muscles are manipulated during the massage, they become relaxed, which improves the range of motion and flexibility.
- Increasing the “feel good” chemical: Massage therapy releases Endorphins, a mood-enhancing chemical that is released in the brain. This “feel good” chemical helps in reducing pain and enhancing recovery.
Prognosis Possibilities
Without treatment or therapy, DDD can gradually progress and cause more adverse symptoms. While surgery is a treatment option, other less invasive treatments such as massage therapy have been found to be just as helpful yet less costly. A clinical study involving a 66-year-old female patient with cervical degenerative disc disease in her lateral left facet joint recorded impressive outcomes. The patient was experiencing symptoms of severe neck pain accompanied by restricted cervical range of motion. She also exhibited radicular left shoulder and arm pain. The objective of the study was to determine the effect of therapeutic massage on the patient’s symptoms and impairments of cervical DDD.
After multiple treatment sessions, the patient’s symptoms had decreased and cervical ROM had moderately improved. There was also a reduction in reported pain and an improvement in functional daily activities. This is an indication that massage therapy is a favorable treatment intervention for DDD symptoms.
Bottom Line
Massage can help improve the symptoms associated with Degenerative Disc Disease for a prolonged duration of time as long as you continue to follow the maintenance schedule that your Massage Therapist lays out. Massage therapy typically reduces muscle strain, improves flexibility, and mitigates pain. However, you can achieve the best results by working in conjunction with other health care professionals. Keep open communication between your doctor and your massage therapist to ensure the best treatment.
To learn about becoming a massage therapist in Seattle contact one of the following local massage schools; Northwest Academy for the Healing Arts or Seattle Clinical Massage School






